The ACL is a strong ligament in the centre of the knee connecting the tibia to the femur. It prevents the tibia from moving forwards excessively on the femur and limits twisting. A tear of the ACL can lead to giving way of the knee during exercise. The ACL is the most commonly torn ligament in the knee.
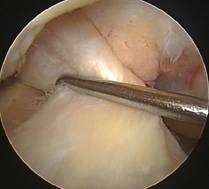
Arthroscopic photo of a normal
right ACL being tested with a small hook
The major cause of an ACL tear is a sporting injury whereby the ligament is overstretched in an abnormal twisting movement or due to a blow to the front of the knee. Common sports during which this can happen include rugby, football, basketball and skiing. However the ACL can also be injured during an awkward landing from a jump or from a sudden change in direction.
The diagnosis of an acute ACL rupture surprisingly is not always easy to make. There are clinical examinations to test the knee’s stability but in a swollen painful knee these can be difficult to carry out. Magnetic resonance imaging (MRI) is now performed routinely to aid diagnosis and even a diagnostic knee arthroscopy may be necessary.
The history or circumstance of the injury is extremely important. More often than not patients hear or feel a loud ‘snap’ at the time of injury. Sometimes even teammates can hear a ‘pop’! This is usually accompanied by pain and a rapid swelling of the knee with an inability to continue the activity. Unfortunately other important structures within the knee are frequently damaged as well including the menisci, the articular cartilage and the collateral ligaments. These can often (but not always) be addressed at the same time as the ACL reconstruction. More than half of all patients with an ACL injury also have a damaged meniscus.
Factors to consider when deciding upon reconstruction of the ACL include
- Age of patient
- Level of pre-injury activity (including sports / recreation)
- Degree of instability / pain / giving way
- Associated damage to other structures
As a general rule physiologically young patients with high demands on the knee require ligament reconstruction. However careful physiotherapy can occasionally be all that is required in some patients with an ACL deficient knee. It is therefore very important that every patient receives physiotherapy as soon as the diagnosis in made whether surgery is planned or not.
Mr Rees is happy to discuss the pros and cons of surgery and indeed the timing of surgery with every patient as the post-operative rehabilitation is extensive and crucial to clinical success. ACL reconstruction is now a highly successful procedure with approximately 90% of patients being able to return to pre-injury level of sporting activities within 9 months.
Surgery
ACL reconstruction is a day case procedure performed under general anaesthesia. Most of the operation is undertaken arthroscopically and through very small skin incisions. The damaged ACL can be replaced by using either the patient’s own hamstring tendons (semitendinosis and gracilis) or the middle third of the patellar tendon which connects the patella to the tibia. More often than not hamstring tendons are used by Mr Rees as these avoid some of the complications that harvesting the patellar tendon can very occasionally cause.
The two hamstring tendons are harvested through a 3cm incision at the top of the tibia on the inside of a right knee.
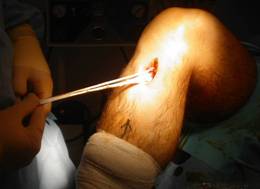
Hamstring tendons being harvested from a right knee
These tendons are then cleaned up and prepared in order to become the ‘new’ ACL. The two tendons are folded in two to make a four stranded graft of between 10-12cm in length and usually 8-10mm in diameter. The rest of the operation is performed arthroscopically.
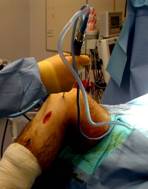
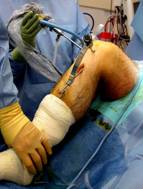
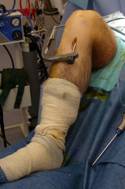
Photos showing arthroscopic ACL reconstruction
The area in the centre of the knee where the ACL used to be is cleared with a shaver. A tunnel whose diameter corresponds to that of the harvested graft is then drilled through the top of the tibia into the centre of the knee. A blind-ended tunnel is also drilled into the lower end of the femur using a special jig to aid the exact positioning of the tunnel.
The prepared graft is then carefully pulled through the tunnels from the lower end up through the tibia into the femoral tunnel using a loop of wire. The new ACL is secured in place with a cross pin in the femur which goes through the loop of the graft and a screw is used to fix the lower end of the graft in the tibia. Both the cross pin and the screw are manufactured from bio-absorbable material and no metalwork is routinely used.
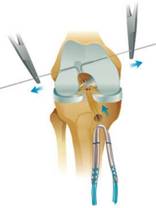
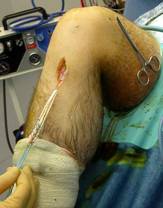
On the left a diagram of the graft being pulled through the tunnels and on the right a peri-operative photo
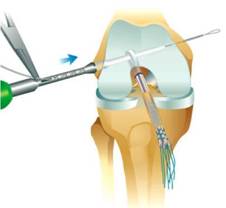
Hamstring graft being fixed in femur by absorbable cross pin
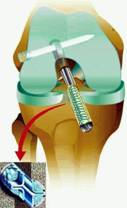
Graft fixed into tibia with absorbable interference screw
With the new ligament firmly fixed the knee is then tested to make sure it is stable. Photographs are taken of the new ligament in place and the knee is washed out. The small incisions are closed with invisible sutures. A wool and crepe bandage is then applied. The whole operation takes approximately 60 to 90 minutes. No brace is normally required.
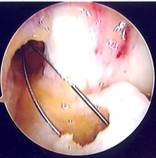
Arthroscopic photo showing the tunnels and the wire loop
traversing the knee with the intact PCL at the back
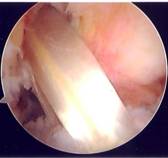
Arthroscopic photo showing the new ACL graft
having
been pulled up through the knee
Back on the ward after the surgery the patient is reviewed by the physiotherapist prior to discharge and given clear instructions with regards to what to do in terms of knee mobilization. Full weight-bearing and unlimited flexion are usually permitted. Hopefully most patients will be feeling well enough to go home the same day but occasionally one overnight stay in hospital is suggested depending on the level of discomfort.
Post-operative rehabilitation
The importance of the physiotherapy after the surgery cannot be understated. It is often the difference between an average and an excellent clinical outcome in some cases. A high degree of motivation and dedication are required from the patient. The total duration of the rehabilitation is between 6 and 9 months and the regime goals are briefly outlined below but there may be variations for individual patients:
- 0-2 days post-surgery
- Mobilise full-weight bearing with crutches
- Early range of movement (knee flexion / extension)
- Basic strengthening exercises
- Advice about ice / elevation / ensure adequate analgesia
- First 2 weeks post-surgery
- First physiotherapy out-patient appointment
- Increase knee strength / range of movement (controlled one leg standing)
- Stretching of hamstring and calf muscles
- Settle pain and swelling
- Prevent adhesions (patello-femoral joint mobilisation)
- Introduce knee stability training
- Gait re-education (walking)
- Discard crutches by end of 2 weeks
- 2 to 6 weeks post-surgery
- Introduce bike (if good flexion)
- Stepping / rowing machine
- Work on balance training / joint awareness
- Aim for normal walking pattern
- Targeted exercises for hamstrings, quads, glutei and calf muscles
- 6 to 12 weeks post-surgery
- Cross-trainer / swimming
- Progressive strengthening / balance exercises (wobble board / trampet)
- Aim for no pain or swelling
- Full range of movement
- 3 to 6 months post-surgery
- Running / technical training
- Deceleration training (hops / jumps / lunges)
- Jogging
- 6 to 9 months post-surgery
- Return to sports specific training
There is a long period of time where the reconstructed knee is much weaker than the other knee. Obviously there is a chance of injury during this period if patients push themselves too hard. Three months post-surgery is often regarded as the transition time to more aggressive activity. This is roughly the time it takes for the body to grow a network of new blood vessels in the graft – this process is known as ‘revascularisation’. When revascularisation is complete graft strength gradually increases.
Complications
Although a vast majority of patients are able to return to their pre-injury level of physical activity, some patients unfortunately may experience some of the complications or recognised problems associated with ACL reconstruction. Such problems include
- surgical wound infection
- lack of full range of movement (especially extension) and stiffness
- weakening of hamstring muscles (although this is usually compensated for)
- bleeding or blood clot in the leg (very rare)
- graft failure due to re-injury, tunnel placement, tensioning or graft-specific factors
- failure or breakage of graft fixation
- persistent instability and pain with an inability to return to previous sporting activity
- some numbness in skin adjacent to small incisions
For a professional athlete an ACL injury even with reconstructive surgery can potentially be a career-ending injury. Fortunately this is not the usual outcome but patients must be aware that a modification of activity following this injury may be inevitable.
