Knee replacement surgery is now a very commonly performed procedure in the UK with approximately 30,000 operations carried out per year. The main reason for requiring an artificial knee is arthritis in the knee. Normally the surfaces of the bones that make up the knee joint are smooth and essentially frictionless but with the onset of arthritis these surfaces become damaged and rough. The cartilage lining wears away and the knee is left with pain, reduced movement and stiffness.
Total knee replacement may help if there is
- Severe pain limiting activities e.g. walking, climbing stairs
- Limited movement or stiffness that stops normal bending of the knee
- Knee deformity e.g. a tendency to be bow-legged or knock-kneed
- Pain at night or at rest or pain that disturbs sleep
- Knee instability or giving way when standing or walking
It is extremely important to have tried all other treatment options for knee arthritis prior to being considered for a replacement. These include weight loss, painkillers (especially anti-inflammatory tablets), physiotherapy, braces or supports and possibly steroid injections into the knee joint. In some patients other forms of surgery may be more appropriate including knee arthroscopy (keyhole washout), osteotomy around the knee (leg straightening) or unicompartmental knee replacement.
Before surgery
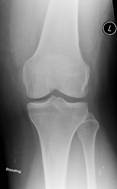
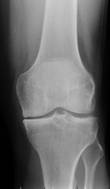
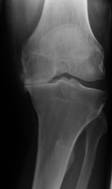
A detailed medical history is undertaken in addition to a thorough physical examination. In particular it is essential to assess the range of movement, straightness, strength and stability of the knee joint. X-rays are performed and these will show the amount of arthritis or damage in the knee. The degree of damage in the knee occasionally determines the type of prostheses to be used.
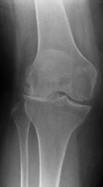
X-rays of three knees – on the left is a normal knee; in the middle there is some early medial osteoarthritic change; on the right there is advanced osteoarthritis with medial compartment collapse
The operation
During the surgery either a spinal or a general anaesthetic will be given. More information can be found in the anaesthesia section. The duration of the surgery will be approximately 90 minutes in total. Intravenous antibiotics are routinely given immediately before and after the surgery to help reduce the risk of infection. A tourniquet is placed around the upper thigh and this has the purpose of stopping the blood flow to the knee during the surgery. The knee is then painted with antiseptic fluids and carefully draped to create an ultra-clean sterile operating field. Much of the operation is carried out with the knee bent up at 90 degrees.
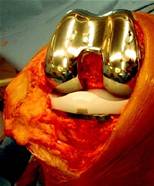
A cut is made over the middle of the knee and is approximately 15-20cm long but this can vary from patient to patient. The kneecap and muscles are carefully moved to one side to expose the knee joint. The damaged bone ends (femur and tibia) are accurately removed with a saw using special jigs as guides depending on the patient’s own anatomy. Measurements are taken to guarantee an excellent fit for the new knee. The artificial joint is then inserted – this is made from highly machined metal (cobalt chrome and titanium) and plastic (polyethylene). Biological cement is used to fix the artificial knee to the bone. During the operation the new knee is bent and rotated to make sure it is stable and moves smoothly.
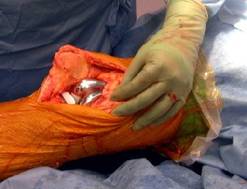
Photograph of artificial knee joint having just been inserted
There are many different types of artificial knees and full explanations will be given before surgery as to why one particular type will be used rather than another. Before closing the wound, a special drain is inserted into the knee to collect blood into a bag. The patient’s own blood can then be given back to the patient through a vein if required. This ‘autologous’ blood transfusion avoids all of the risks that receiving donated blood can cause.
Photograph of implants with knee out fully straight
The muscle layers are carefully brought together with strong dissolvable sutures and the skin is then closed up with metal clips. Immediately after the operation the patient is wheeled to a recovery area for a short while before returning to the ward.
A thick wool and crepe bandage is applied to the knee and this stays in place for no more than 24 hours. The drain is also removed at the same time on the ward.
After surgery
The first day after the surgery the patient is seen by specialist physiotherapists who encourage the patient to sit out of bed in a chair and commence full weight bearing with the aid of crutches. Two critical goals to be achieved prior to leaving hospital are the ability to get the knee fully straight (full extension) and the ability to bend the knee to at least 90 degrees. It will be somewhat painful moving the knee so soon after surgery but experience has told us that early movement is very beneficial for a favourable long-term outcome. Of course strong painkillers are routinely administered during this period. The physiotherapists will visit the patient on a daily basis but the patient will be responsible for carrying out regular exercises on their own during the day as instructed by their physiotherapist.
Most patients stay in hospital between 3 and 6 days after the surgery but no-one is discharged unless they are competent and confident at walking, have gone up and down some steps and the wound is dry and healing well. Every patient also has post-operative check x-rays of the knee and blood tests to make sure they are fit and well enough to go home. In order to minimise the risk of developing a blood clot, every patient wears foot pumps which intermittently squeeze the feet to maintain blood flow back to the heart and also receives a blood thinning injection into the tummy (low molecular weight heparin). Compression stockings (TEDS – thromboembolic deterrent stockings) are also used to encourage blood flow in the legs.
At home
When patients arrive home they will be able to move around the house and manage stairs. Occasionally the Occupational Therapists will be involved in overseeing a patient’s discharge from hospital – their role is to make the patient’s home safer and easier to navigate immediately after the surgery. This may involve the installation of handrails along stairs or in the shower, arranging toilet seat raises and footstools etc.
It is essential that patients continue with the knee-strengthening exercises outlined to them during their hospital stay. These need to be performed several times a day. The patient will also receive instructions about wound care. Approximately twelve days after the operation the clips will be removed usually by a practice nurse. It is likely that the physiotherapists will organise some outpatient appointments to ensure progress with regard to walking and moving the knee is being made.
It may well be a few weeks until the patient can safely go shopping and hence arrangements for friends and family to help out should be made. Driving is not permitted for at least six weeks post-operatively and a return to work date will depend on the nature of the work but will be discussed in detail prior to the surgery. After six weeks Mr Rees reviews all his patients himself. Improvements in knee function commonly occur for up to a year after surgery. Most patients however generally resume most daily activities after 6-8 weeks following the surgery. Patients are able to enjoy a variety of low-impact activities after a knee replacement such as walking, cycling, golf and swimming but other sports which involve running, jumping or contact may be considered as too risky – a full run down of possible limitations will be covered in the pre-operative consultation.
Risks of total knee replacement
Total knee replacement is a major procedure. As with any form of major surgery it carries risks of serious infection, heart attack and stroke. There are also risks of developing thromboembolism (blood clot) including deep vein thrombosis (DVT) and more seriously pulmonary embolism (PE) – a blood clot in the lung. The risk of a serious PE is in the range of 0.1% to 0.5%. The risk of a DVT in the leg or calf is more common but every effort is made to minimise this risk. As mentioned earlier blood-thinning injections are routinely given along with foot-pumps to help push blood back to the heart and the importance of early mobilisation cannot be understated. Adequate post-operative hydration is also critical to keeping the risk of developing a blood clot down.
Increased risk factors for DVT development include
- Age over 40 years
- Obesity
- Pre-existing venous problems (varicose veins)
- Smoking
- Diabetes
- Coronary artery disease
- Previous history of DVT
Clearly, losing excess weight and stopping smoking prior to surgery are two major beneficial actions that patients can undertake to make knee replacement surgery more successful and diminish post-operative complications.
Infection of the knee itself can cause persistent pain, swelling and loss of function. It can ultimately lead to loosening and failure of the knee replacement. Infection needs to be treated aggressively and swiftly but proven infection frequently demands further major surgery to exchange the components to eradicate it. The risk of infection following knee replacement is approximately 1%. To minimise infection risk intravenous antibiotics are given just before and after surgery. Meticulous hand washing, careful wound care and ultra-clean air theatres are other critical measures that make the risk of serious infection very low.
Other risks of knee replacement include damage to nerves around the knee leading to weakness, numbness or pain in the leg or foot (<0.5%) and damage to blood vessels behind the knee (<0.2%). If circulation to the leg is compromised during surgery then further emergency surgery to restore the blood flow is carried out. Fortunately these complications are extremely rare.
Knee replacement technology is constantly improving and 95% of modern knees should last at least 15 years and hopefully longer. However occasionally a knee replacement can wear out or ‘fail’ prematurely. If this is the case a second or revision knee replacement will be required.
Despite possible complications following knee replacement the vast majority of these operations result in an excellent outcome. More than 95% of patients undergoing total knee replacement enjoy significant pain relief, better mobility and an improved quality of life.
X-ray gallery
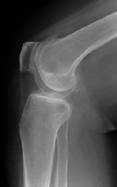
Pre-operative x-rays of an arthritic valgus right knee
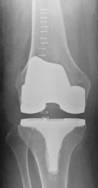
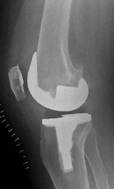
Post-operative x-rays of the same knee showing the new knee replacement
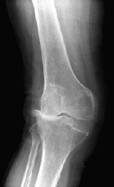
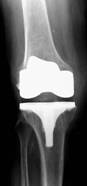
Pre and post-operative x-rays showing a very arthritic valgus
right knee to be much straighter after surgery
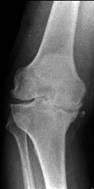
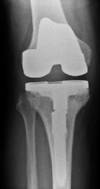
Pre and post-operative x-rays of a varus right knee with
tibial bone loss requiring a stemmed tibial insert
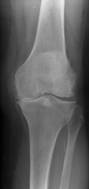
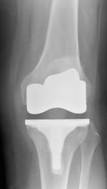
Pre and post-operative x-rays of left knee with medial
osteoarthritis
with standard total knee replacement