Apart from ligaments and menisci, the actual smooth surface of the bone ends in the knee joint can be injured and damaged. Commonly this occurs after a heavy fall or direct impact of the femur on the tibia. The articular cartilage has very poor regenerative capabilities and once damaged never really recovers to its pre-injury state.
Cartilage damage can cause persistent pain and instability in the knee and ultimately is a pre-arthritic condition. Significant research is being undertaken to investigate new ways of transplanting or regenerating cartilage. Mr Rees is one of only a handful of surgeons in the UK who has been trained in these new techniques and is currently undertaking cartilage transplantation surgery. All such surgery closely follows guidelines as established by NICE regarding its use and research protocols.
The actual procedure involves two separate operations. The first involves a day case knee arthroscopy during which the cartilage defect is visualised. The defect is usually on the femur but can be located on the undersurface of the patella or kneecap. The defect has to have certain characteristics in order for the procedure to be suitable in terms of its size (less than 10cm2) and exact location. A very small biopsy of undamaged cartilage is taken from the side of the knee in an area that will not compromise the knee’s function.
The biopsy is then immediately transferred into a transport container and sent to a laboratory in Austria where the biopsy is mixed with a liquid collagen matrix (the protein building blocks of cartilage) and incubated for two weeks. A transplant (the new cartilage) is then formed and is fully adjustable in size and thickness to suit the exact defect in the injured knee.
At the second operation the knee is opened to expose the defect, which is prepared, and the edges freshened up. The tailor-made transplant is then attached with biological glue called fibrin glue onto the base of the cartilage defect. The operation usually takes about one hour. It will involve a 1-2 day stay in hospital.
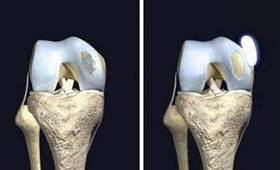
Area of damaged area of cartilage on the left and
on the right a ‘transplant’ ready to be inserted
Immediately after the surgery the leg is placed into a brace and rested for 48 hours. After this time continuous passive motion is commenced. Full extension is permitted but flexion is restricted to sixty degrees. Only slight weight bearing is allowed (15-30kg) for the first four weeks after surgery. Careful physiotherapy is undertaken and full movement can occur after six weeks but full weight bearing is not recommended until six to twelve weeks post surgery in order to allow the transplant to fully incorporate. It is also suggested that sporting activities be avoided for up to 6 months.
It must be stressed that cartilage transplantation remains experimental and ongoing research is essential. Early results however appear to be favourable and in one particular study approximately 80% patients reported very good results one year after the surgery.
