Although the majority of Mr Rees’ surgical workload comprises the treatment of knee disorders, he also carries out between 60-80 total hip replacements per year. Mr Rees received extensive instruction in hip replacement surgery while working on the Joint Reconstruction Unit at the Royal National Orthopaedic Hospital, Stanmore as part of his specialist training. He is now one of the main hip replacement surgeons at Broomfield Hospital.
The hip joint is a large ball and socket joint and similar to the knee unfortunately is prone to the development of painful osteoarthritis. The hip joint comprises the acetabulum (socket) and the femoral head (ball).
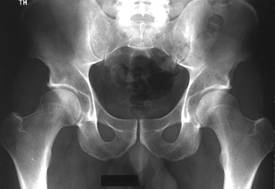
Pelvic x-ray showing normal hip joints
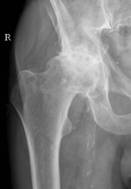
X-ray of very arthritic right hip joint with bone rubbing on bone
Again, like the knee joint, there is a smooth essentially frictionless covering of the bones of the hip joint made of articular cartilage. When this wears down patients describe groin pain, lateral thigh pain, restricted hip movement, stiffness and sometimes a limp.
When established osteoarthritis is seen on x-ray, a total hip replacement may well be required. However, prior to such surgery it is important for a patient to receive hip strengthening physiotherapy, to try using a walking stick (this can offload the force transmitted through the hip joint) and to be prescribed anti-inflammatory painkillers. In addition, especially in the younger patient, an injection of steroid into the hip under x-ray control may well have been carried out. Such an injection can also be very helpful to differentiate between genuine hip pain and pain coming from an arthritic lower back which frequently presents like hip arthritis.
When the decision has been made to proceed to surgery, every patient will be medically assessed and advice given regarding the most appropriate type of anaesthetic. Further information can be found in the anaesthesia section. These anaesthetic choices are identical for patients undergoing either hip or knee replacement surgery.
For the operation the patient lies on their side with low back and pubic supports. Mr Rees carries out total hip replacement surgery through a single lateral mini-incision of between 10-12 cm long. During the operation some of the muscles around the hip are carefully reflected out of the way and great care is taken to reconstruct them when closing the wound. The worn out femoral head is dislocated from its socket and the top of the femur is cut. The socket is then prepared and an artificial metal acetabular shell is inserted usually without cement into the pelvis and occasionally the fixation is supplemented by screws. A polyethylene liner is then snapped into the shell offering a very durable bearing surface. The top of the femur is hollowed out to receive a femoral prosthesis (either cemented or uncemented).


Model of normal femur on the left but with the neck cut
and a femoral prosthesis in situ on the right
A femoral head is then attached to the prosthesis and this is made of cobalt chrome, ceramic or oxinium. The new hip is reduced and a very careful assessment is made of the hip’s stability, its range of movement and leg length equality. The wound is then meticulously closed and one deep drain is left in place for 24 hours. The skin is closed with clips and the wound covered by a spirit-soaked gauze. A wool pad is then taped over the gauze. As with knee replacement intravenous antibiotics are given immediately before and after the operation.
The operation takes between 60-90 minutes on average. Patients are encouraged to get up full weight bearing on the first post-operative day. The inpatient hospital stay is usually between 3 and 6 days and during this time the patient receives injections to thin the blood and compression foot pumps to decrease the risk of a blood clot forming. A routine post-operative blood test and check x-ray are carried out. Occasionally a blood transfusion is required after a hip replacement. Physiotherapists review patients regularly prior to discharge to educate patients as to what range of movement of the new hip is safe immediately after the surgery. Outpatient physiotherapy will also be organised. No driving is permitted for 6 weeks after surgery and it does take up to 6 months for the muscles around the hip to reach their pre-operative strength. Mr Rees reviews all patients 6 weeks after their hip replacement and thereafter at regular intervals.
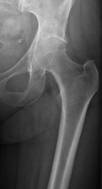
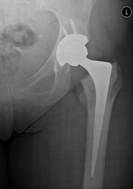
Pre and post-operative x-rays of a left hybrid total hip replacement
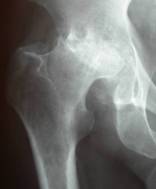
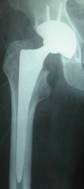
Pre and post-operative x-rays of a right uncemented total hip replacement
As with any major orthopaedic surgery there are risks associated with hip replacement. The risks are small but real and include the following
- Infection
- Nerve damage
- Bleeding
- Blood clot (DVT)
- Dislocation
- Early loosening
- Leg length difference
Just under 70,000 hip replacements are carried out in the United Kingdom each year and the contribution of this operation to improve a patient’s quality of life is arguably unparalleled. There are numerous different types of hip prostheses and Mr Rees will be happy to discuss the types available. A modern day hip replacement should last between 10 and 15 years. After this time a revision type procedure may be required if the hip has become loose or the bearing surfaces have worn out.
Please note that Mr Rees does not carry out hip resurfacing or complex revision hip replacement surgery. However he does offer uncemented hip replacement and large metal on metal bearing surfaces for the younger patient with an arthritic hip. Mr Rees would be more than happy to fully assess any patient with a painful hip and recommend appropriate colleagues who may be able to offer a more suitable operation if required.
